At least 15% of American adults suffer from moderate-to-severe headaches. The cause is multi-factorial and can be triggered by many things, including:
- Brain injury/concussion
- Poor quality of sleep and/or poor sleep posture (i.e. not supporting your head in a neutral alignment while sleeping)
- Poor posture (slouching while sitting at your computer, constantly looking down at your cell phone)
- Dehydration
- Eating sugar and other dietary aggravators (processed food, alcohol, caffeine)
- Fluctuations in hormone levels (menstrual cycle, menopause)
- Many other factors.
A headache can be indicative of a serious medical emergency. For example, the ‘sudden onset of the worst headache of your life’ may be indicative of a brain hemorrhage (stroke). If this describes your headache, stop reading this and go to the hospital! Constant pain and tenderness at the temple on one side of your head may be indicative of a condition called temporal arteritis – this, too, requires medical attention. While the vast majority of headaches are not life-threatening, all headaches significantly affect the quality of life of the sufferer and his/her loved ones.

Photo by Alexander Krivitskiy on Unsplash
Diagnostically, there are at least four categories of headache:
- Migraine
- Tension-type
- Cluster
- Cervicogenic
Each of these categories is characterized by variable signs and symptoms – some of which overlap and some of which are distinct. There is also significant overlap in causality amongst these diagnostic categories. Recognizing that the cause is multi-factorial, one of the most significant contributors to headache pain is upper cervical spine (upper neck) dysfunction.
A Brief Lesson in the Neurophysiology of Headaches (I’ll try to keep it simple)
It is well-documented that each diagnostic category of headache involves, to some degree, the Trigeminal Nerve (Cranial Nerve V). The most current theory regarding the physiology of headaches is that some degree of inflammation causes the Trigeminal Nerve to initiate a depolarization of cortical brain activity and/or dilation of cranial blood vessels. Note it is a theory and we aren’t exactly sure of the cause(s). Hang in there, because this is where it gets exciting… All information that is gathered/sensed/perceived by the Trigeminal Nerve is processed in the Trigeminocervical Nucleus (TCN) before being relayed up to the brain for further processing. This nucleus is a region of the upper cervical spinal cord (C1-C3). Therefore, there is a cervical spine component of all headaches. The TCN also processes lots of information from the head and face (Facial Nerve – Cranial Nerve VII, Hypoglossal Nerve – Cranial Nerve XII, Vagus Nerve – Cranial Nerve X), and the spinal nerves from the upper cervical spine (C1-C3). This means that information from all of these sources – including the ligaments, facets, discs, and muscles of the upper cervical spine – must pass through the TCN for processing. As this convergence of incoming signals is processed by the TCN and higher brain centers, the exact source of certain sensations may be misinterpreted. This means that a strained muscle in your neck may send messages, such as ‘danger’ or ‘inflammation’, to your TCN and then on to your brain, but your brain may perceive this information to be coming from your head, not your neck. Thus, you have a cervicogenic headache. This misinterpretation of sensory input/output is called referred pain, and you can read more about it here.
Stop Suffering from Headaches:
To summarize what we’ve covered so far:
- There are many causes and various diagnostic categories for headaches
- The physiology of headaches is complex, but clearly implicates the upper cervical spine as a primary contributor to headache pain
There is also a great deal that can be done to resolve headaches. My colleagues and I have helped many people overcome headaches through two simple steps:
- Identify triggers and ‘stop picking the scab’
- Improve your neck mobility and strength
Identify Triggers and Stop Picking the Scab
In order to heal, you must identify aggravating factors and avoid those things that are increasing strain and inflammation. Below are three of the most common triggers I see, and some simple solutions.
- Sleep posture: This is important for everyone, but especially for those of you who wake up with a headache. If you are a stomach sleeper, STOP sleeping on your stomach. This puts too much pressure/tension on the neck, as your neck is forced into rotation. Instead, sleep on your back or your side. If sleeping on your side make sure that the pillow you use is thick enough (but not too thick) to support your neck in a neutral position. Your head should not be tilted up or down but should lie flat. For more detailed information on how to support yourself to get a good nights sleep, read this.
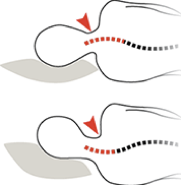
Examples of over-support and under-support
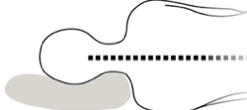
Example of pillow assisting to keep head/neck neutral
- Neck posture: I have had many clients whose primary trigger was looking down for prolonged periods of time. Whether you are looking at your cell phone, reading a book on the train, or falling asleep on a plane, this places tremendous strain on the muscles and passive structures of your neck. Remember, this ‘strain’ is relayed through the Trigemino-cervical Nucleus and up to the brain. The brain may misinterpret the source of the information and perceive neck strain as headache pain. So, keep your head aligned over your shoulders and hold your phone/book up to a level that doesn’t strain your neck. Even better, support your arms using armrests or a pillow on your lap so that you can more easily maintain this position without straining your shoulders.
- Diet and Hydration: I have also had many clients whose trigger was related to their diet. Sugar is often times a culprit. Keep in mind that simple carbohydrates, like bread, are ‘sugar in disguise’ (eating 2 slices of whole grain bread is equivalent to eating up to 10 teaspoons of sugar because of how our body converts these simple carbs into glucose!). Do you tend to get a headache after indulging in sugar/processed food? If so, it is in your best interest to avoid sugar and all processed foods.
- Dehydration can also contribute to headaches. A good goal is to consume 1 Liter of water for every 1,000 calories you consume. Most people do not drink enough water.
Improve Your Neck Mobility and Strength
As outlined above, the neck is often times implicated in headaches. Stiffness and/or weakness of the joints and muscles of the neck is a primary factor in susceptibility to headaches and neck pain in general. It is best to consult with a IPA physiotherapist to identify and address your specific needs. We are skilled in various manual therapy techniques, such as soft tissue/fascial mobilization and joint mobilization/manipulation, that are highly effective in the treatment of headaches. That being said, I commonly prescribe the following exercises to help treat headache pain. Try them out and evaluate if they are effective for you. If you experience a worsening of symptoms, stop and consult a physio.
Yoga strap neck stretch
- Begin by draping the yoga strap over the top of the shoulder to be stretched. The strap should be anchored under the opposite foot (one end of the strap under the forefoot, with the strap continuing under the foot). Keep the heel lifted.
- Hold the strap in front with the hand of the side that is not being stretched. Gently pull down to engaged mild-moderate (start with mild) tension.
- Lower the heel to the ground, increasing tension in the strap.
- Maintaining the tension from the strap, perform the following neck motions in a slow and controlled manner. Hold each stretch for 5-10 seconds, then return to mid-line before continuing further.
- Look down
- Rotate to the side opposite the strap
- Look down and towards your armpit
- Tilt head to the side
Supine axial elongation with self-resisted neck flexion and long-neck extension
- Lie on back in hook-lying position.
- Place one hand under the occipital and upper cervical region and the opposite thumb under the chin.
- Resist the head and neck pressing into the floor while resisting an isometric contraction of the chin tuck.
It is my sincere hope that having a better understanding of the mechanisms of headaches and a practical game plan to address your unique contributing factors will resolve your pain. If you have any questions please leave a comment. Thank you for reading!
References:
Bogduk N. Anatomy and Physiology of Headache. Biomedicine and Pharmacotherapy 1995, Vol. 49, No. 10, 435-445.
Headache and vertigo of cervical origin. Elsevier: 2013. *cited as Elsevier, 2013[p’;;/q1
Howard PD et al. Manual Examination in the diagnosis of cervicogenic headache: a systematic literature review. JMMT. 2015;vol 23;no.4; pp210-218.