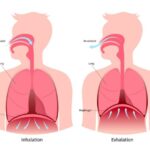
Myofascial Decompression (MFD), or ‘cupping’, has been around for thousands of years. Recently it has re-gained popularity within the health and wellness community and amongst physical therapy professionals. So, besides leaving red circles on the skin, what is the point?
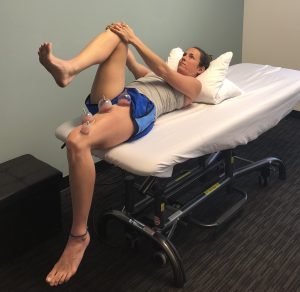
MFD is unique amongst manual therapy modalities in that it is, by nature, decompressive. Most manual therapies are compressive in nature – be it soft tissue mobilization (STM) / massage or joint mobilization / manipulation (JM). During STM and JM pressure is placed into the body in an attempt to enhance mobility of the soft tissues or joints. During MFD, negative pressure created by the suction draws the skin and fascial layers away from the midline of the body. This decompression alters blood flow and metabolic exchange within the tissues.
MFD has been shown to be as or more effective at improving flexibility and decreasing pain than heat, stretching, and foam rolling. Muscle pain and tenderness is often related to decreased blood flow, which leads to an increase of metabolic by-products like lactic acid. MFD helps draw toxins out of muscles and to the superficial veins to be removed by the body. This leads to decreased pain and decreased tension in the tissues. MFD may enhance mobility through affecting fascial adhesions, tissue temperature, and viscosity of tissues (lubrication).
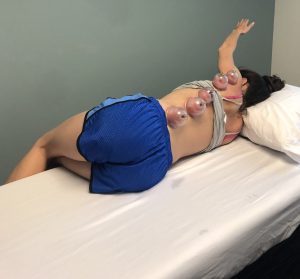
MFD decreases pain by eliciting the release of endorphins and altering pain thresholds.
Research will continue to highlight mechanisms for how MFD works. Clinically, there is no doubt that it is a great tool to manage soft tissue dysfunction. Our clinical experience indicates that MFD is most effective as part of a thorough plan of care – including soft tissue mobilization, joint mobilization, neuromuscular re-education, and exercise.
References
- Daprato, C. Effects of Soft Tissue Mobilization With Negative Pressure Device on the Shoulder, Using MR Imaging.
- Kim et al. Effect of Cupping Therapy on Range of Motion, Pain Threshold, and Muscle Activity of the Hamstring Muscle Compared to Passive Stretching. J Korean Soc Phys Med, 2017; 12(3): 23-32
- Yim et al. Comparison of the effects of muscle stretching exercises and cupping therapy on pain thresholds, cervical range of motion and angle: a cross-over study. Phys Ther Rehabil Sci, 2017, 6 (2), 83-89