A tendinopathy is a term to describe pain, swelling, and functional impairment to a tendon. Photobiomodulation (also knowns as cold laser therapy) has been shown to treat the symptoms in both tendinitis and tendinosis, as well as performing as a reliable adjunct in the rehabilitative process. The intention of this article is to shed some light on how photobiomodulation can help heal the damaged tissue. Additionally, clarity will be introduced on how tendinitis differs from tendinosis.
Tendinitis
Tendinitis is less common, and is the appropriate diagnosis when there is a recent injury causing a sudden spike of inflammation in a tendon. Symptoms of pain, heat, stiffness, swelling, and limited tolerance to activity are typical and last in a range of 2- 10 days. However, some cases have been known to persist. Photobiomodulation is the ideal treatment to heal the damaged tissues that caused tendon inflammation.

The primary benefits that photobiomodulation brings to the table are the following:
- Stimulation of collagen production from tendon cells (tenocytes)
- Immune system damage control
- Muscle tissue repair by stimulating muscle regenerating stem cells!
Immune system damage control involves reigning in the “pro-Inflammatory” (inflammation producing) cells and deploying the “anti-inflammatory” cells. Pro-inflammatory cells are initially helpful to control infection and stabilize the damaged tissue. Resolving this process quickly is ideal in most situations, reducing the likelihood of a stalled or delayed healing process.
What About Tendinosis?
Repeated bouts of tendinitis are an indication that the tendon has never fully healed and is functioning in a degenerative state. This is called tendinosis. Research has shown that in this state, there are actually very few inflammatory cells present in the tissue. Although you might think your tendon is swollen, in reality it isn’t.
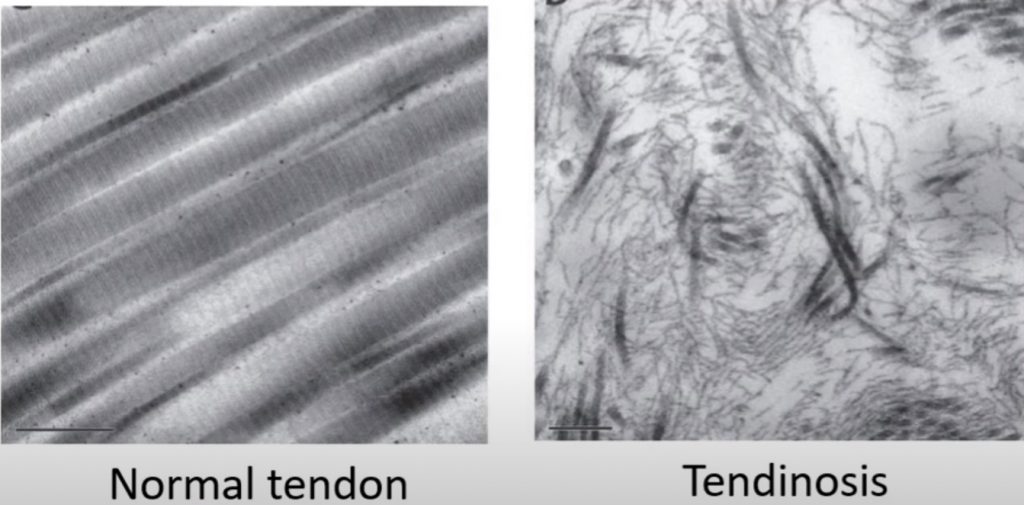
Symptoms of tendinosis usually include stiffness in the morning or after periods of immobility, and dull, aching pain with occasional sharp pain with activity. Healing timelines for tendinosis can be anywhere from 3-6 months on average. This is dependent on the extent of degeneration and whether or not a rehabilitation program has been initiated.
The body heals a tendon by laying down type 3 collagen fibers (the fibers on the right picture). This is a weaker less durable fiber that requires eccentric loading exercises to mature and remodel into stronger type 1 collagen fibers (the fibers on the left picture). Photobiomodulation has been shown to stimulate tendon cells (tenocytes) to produce type 1 collagen (strong organized collagen fiber) vs type 3 (weak disorganized collagen fiber) in tendon degenerative states. This process accelerates recovery and provides stronger tissues.
Eccentric Exercise to the Rescue!
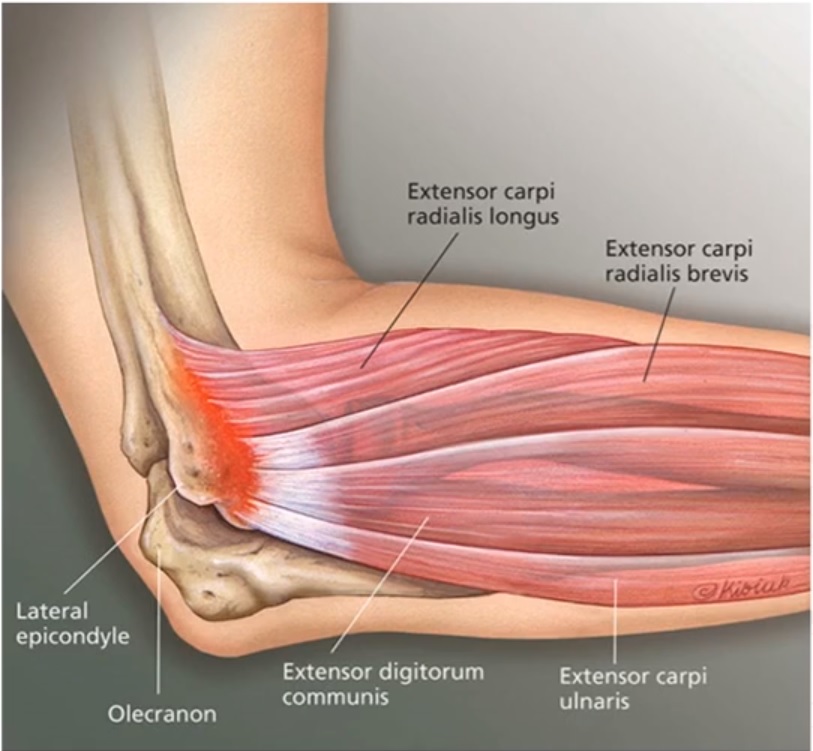
Eccentric exercise causes mechanical stress to the musculotendinous junction. The what? This is the point where the muscle attaches to the bone. In the case of the lateral elbow, the extensor carpi radialis brevis muscle (the most common muscle involved in lateral epiondilytis) attaches to the humerous bone on the lateral epicondyle. Lengthening the muscle under controlled tension (eccentric exercise) pulls tension on the disorganized type 3 collagen fibers, stimulating protein synthesis. This further assists in altering the strength of the collagen into a stronger more resilient type 1 collagen structure. Your clinician at IPA Physio will work with you on safe and effective exercises using the FMT approach. This process is initiated after inflammatory signs and symptoms have resolved.
Don’t Just Mask Pain!
Non-steroidal anti-inflammatory drugs (NSAID) and steroid injections are capable of controlling the pain in both situations. Unfortunately, these drugs have been proven to accelerate the degenerative process within a tendon! This increases the likelihood of more severe injuries such as large tears or ruptures. Photobiomodulation (cold laser therapy) has a curative effect on the tissue and has been shown to be as effective at controlling inflammation in the “itis” phase as well as accelerating the restoration of the degenerative tendon. This is all without any negative side effects!
Get Started Healing!
Currently, photobiomodulation is only available at the IPA Physio Portland location. IPA Physio Portland utilizes the BioFlex laser therapy system to treat and cure a variety of musculoskeletal injuries. These include post surgical, acute sprains and strains as well as chronic degenerative conditions throughout the entire body.
Reach out to IPA Physio Portland for more information on how photobiomodulation can help you!
Articles:
- Comparison of Photobiomodulation and Anti-Inflammatory Drugs on Tissue Repair on Collagenase-Induced Achilles Tendon Inflammation in Rats
- Clinical management of tendinopathy: A systematic review of systematic reviews evaluating the effectiveness of tendinopathy treatments
- A randomised, placebo controlled trial of low level laser therapy for activated Achilles tendinitis with microdialysis measurement of peritendinous prostaglandin E2 concentrations
- Effects of Low-Level Laser Therapy and Eccentric Exercises in the Treatment of Recreational Athletes with Chronic Achilles Tendinopathy