Photobiomodulation (PBM) and platelet rich plasma (PRP) are two well researched and effective forms of regenerative medicine, praised for their ability to repair and heal the body. Painful and debilitating conditions that were once managed through long-term, ongoing medication such as opioids, steroids or NSAIDs can now be targeted and treated through regenerative medicine techniques. Analgesics mask the pain from an injury and NSAIDs interrupt the healing cascade associated with inflammation, each of which can accelerate degenerative changes and sustain disability. PBM and PRP each have proved to promote healing factors in cells when studied in isolation, but research shows the effectiveness of their results are enhanced when they are combined.
Photobiomodulation (PBM)
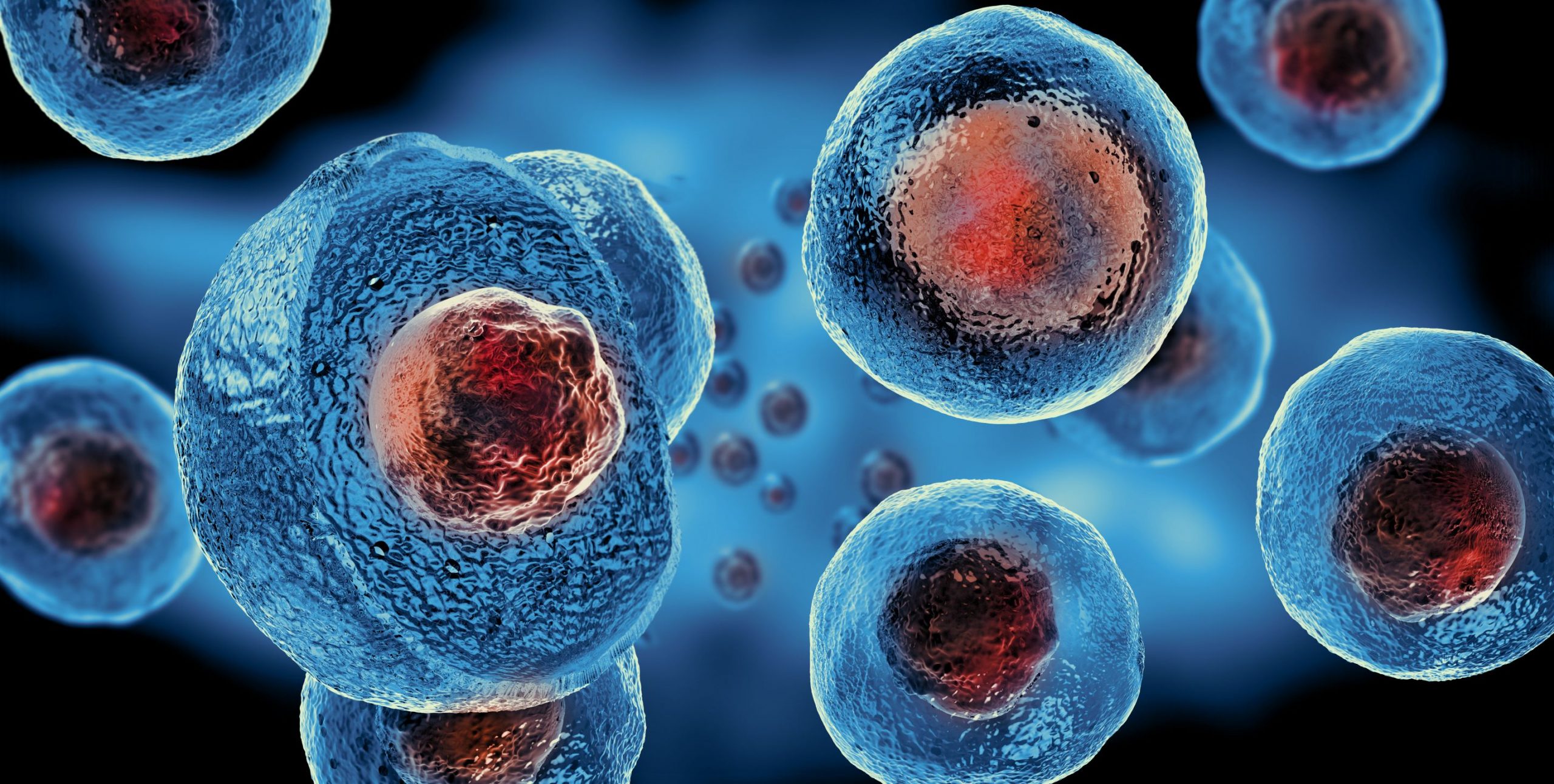
Photobiomodulation is a form of non-thermal light therapy that targets the mitochondria in cells to trigger a cascade of biochemical effects. Mitochondria are the energy producing factories of our cells. These factories are often running on low power due to pain, inflammation, chemical stress, or other suppressive factors affecting production. Specifically the wavelengths of red and infrared light between 660 nm and 840 nm are easily absorbed by cells and have been shown to accelerate the healing cascade in the body through enhanced ATP (the primary source of cellular fuel) production. The benefits are extensive and include reduced oxidative stress, improved collagen synthesis, improved vascularization and acceleration of the inflammation process.
Credit: Bioflex Laser Therapy
Platelet Rich Plasma (PRP)
Platelet rich plasma (PRP) injections utilize the healing power of our platelets to kick start the inflammatory process. Platelets are a type of blood cell that are important for blood clotting, but also are involved in the healing process. Blood is drawn and spun in a centrifuge to separate the platelets and plasma from the other components of the blood, such as red and white blood cells. Plasma is the nutrient rich liquid that our blood cells float in. A concentrated dose of platelets and plasma is then injected into the area of injury or tissue damage. Some physicians will combine the platelets with additives which may enhance the PRP’s regenerative effects.
The platelets themselves don’t heal the body, but stimulate growth factor proliferation in the treated tissues. Growth factors trigger the body to heal itself. There are 2 main variations of PRP: red in color or leukocyte rich, and amber in color or leukocyte poor. The colors are an indication of the amount of white blood cells in the solution. The higher amount of white blood cells in the injection can be an indicator of how much inflammation will be present and experienced by the patient during their post injection recovery. Physicians guide the injections to the target tissue using ultrasound imaging. There is not just one recipe for PRP, and each doctor may have their own recipe or technique based on their equipment, clinical experience, desired outcome, and patient characteristics.
Inflammation is a Good Thing, But Not for Too Long
When damage has occurred, the healing cascade is initiated by the inflammatory response. Inflammation is normal, is intended to last 1-3 days, and is characterized by swelling, heat, redness and pain. The goals of the inflammatory stage are as follows: control the damage, prevent the spread of infection, kill the dying cells, remove the dead tissue, as well as attract the necessary cells the body will use to rebuild and heal the damaged area.
One of the primary cell regulators of this healing cascade is a cell called a macrophage. The macrophage is a type of white blood cell. It serves many roles in the healing cascade, and is particularly active in the inflammatory phase. During the initiation stages of inflammation the macrophage serves two roles, to break down the diseased or damaged tissues (literally by eating them) and releasing pro-inflammatory chemicals. In this state, the macrophage is defined as pro-inflammatory and is called an M1 macrophage.
In the normal response, the inflammatory phase gradually comes to an end while the injured tissue actively begins repairing itself. This process of halting inflammation is strongly dependent on the activity of the macrophage. Normal chemical changes signal the macrophages to convert from pro inflammatory to anti inflammatory cells, also called M2 macrophages. A delayed transition from a pro-inflammatory M1 macrophage to an anti-inflammatory M2 macrophage will delay wound repair.
Pro-inflammatory M1 macrophages remain active in degenerative tissues such as tendinopathy and arthritis. In these cases, it can be hypothesized that the chemistry of the damaged area prevents the normal conversion of the M1 macrophage to the M2 type cell. A consequence of sustained M1 activity is that healthy cells in the region can also be destroyed, when otherwise would be left alone. This results in a sustained degenerative cascade leading to a cycle of perpetual inflammation and tissue breakdown.
PRP has been shown to improve the quantity of M2 anti-inflammatory macrophages in treated tissues. PBM has been shown to increase the transition from M1 pro-inflammatory macrophages to tissue regenerating and repairing M2 cells as well as improve the efficiency at which the M2 cells operate! The result is that you break the vicious cycle of breakdown and degeneration, restoring the body to a balanced state.
Recap: When PRP and PBM are combined they are able to produce more M2 macrophages and improve the speed at which M1 converts to M2. PBM improves the efficiency at which the M2 macrophages operate.
Build Stronger Tendons with Type 1 Collagen
The beneficial effects of PBM and PRP extend into the proliferative stage of healing and beyond. A primary example is through the production and enhancement of collagen. Collagen is the most abundant protein in the body, and makes up more than 80% of the dry weight of tendon.
In numerous studies, PBM and PRP have been shown to improve the production and synthesis of type 1 collagen (a strong, mature collagen variation) in injuries. Type 1 collagen is typically more desirable due it’s stronger structure, and is the dominant type of collagen in healthy adult tendons. One study in 2012 found that PBM and PRP both accelerated the production of type 1 collagen fibers suggesting faster healing of a damaged tendon. Type 3 collagen fibers (disorganized and more fragile) were found to be more frequent in the untreated groups. PBM and PRP alone proved to be significantly more effective than no treatment, but when combined the results were superior.
Another study performed in 2016 found that when rats who had calf strains were treated with PBM, they demonstrated reduced inflammation, more cellular regeneration, reduction in oxidative stress and improved collagen orientation and thickness after 7 days of daily treatment. They performed PRP injections to a second group of rats with calf strains and found similar results with reduction in inflammation between the cells and improved amounts of regeneration of cells. When the third group was treated with both PBM and PRP, even better results were identified, showing a greater number of cells in regeneration, greater presence of blood vessels, a lower area of injury and healthier muscle fiber orientation. Once again, the combination of PRP and PBM produced superior results.
Grand Finale
Making the choice between which intervention to pursue can be challenging, and can be often limited to availability and access to services. Whether you have had platelet rich plasma injections or photobiomodulation, addressing applicable mechanical, neuromuscular, and motor control dysfunctions are critical to restore your functional efficiency. Currently, photobiomodulation is only available at the IPA Physio Portland location. IPA Physio Portland utilizes the BioFlex laser therapy system to treat a variety of tissue injuries. These include post surgical, acute sprains and strains as well as chronic degenerative conditions throughout the entire body.
With a complimentary phone consultation we can help answer any questions you might have, and whether your injury is one that will likely respond well to PBM.
Reach out to IPA Physio Portland for more information on how photobiomodulation can help you!
Research Articles
Tomazoni, S. S., Leal-Junior, E. C., Frigo, L., Pallotta, R. C., Teixeira, S., de Almeida, P., Bjordal, J. M., & Lopes-Martins, R. Á. (2016). Isolated and combined effects of photobiomodulation therapy, topical nonsteroidal anti-inflammatory drugs, and physical activity in the treatment of osteoarthritis induced by papain. Journal of biomedical optics, 21(10), 108001. https://doi.org/10.1117/1.JBO.21.10.108001
Hamblin M. R. (2017). Mechanisms and applications of the anti-inflammatory effects of photobiomodulation. AIMS biophysics, 4(3), 337–361. https://doi.org/10.3934/biophy.2017.3.337
Centeno, C., MD. (2019, September 17). Considering a PRP Injection? Please Read This. . .. Regenexx. https://regenexx.com/blog/prp-injection/
Souza, N. H. C., Mesquita‐Ferrari, R. A., Rodrigues, M. F. S. D., Silva, D. F. T., Ribeiro, B. G., Alves, A. N., Garcia, M. P., Nunes, F. D., Silva Junior, E. M., França, C. M., Bussadori, S. K., & Fernandes, K. P. S. (2018). Photobiomodulation and different macrophages phenotypes during muscle tissue repair. Journal of Cellular and Molecular Medicine, 22(10), 4922–4934. https://doi.org/10.1111/jcmm.13757
Nishio, H., Saita, Y., Kobayashi, Y., Takaku, T., Fukusato, S., Uchino, S., Wakayama, T., Ikeda, H., & Kaneko, K. (2020). Platelet-rich plasma promotes recruitment of macrophages in the process of tendon healing. Regenerative therapy, 14, 262–270. https://doi.org/10.1016/j.reth.2020.03.009
Landén, N. X., Li, D., & Ståhle, M. (2016). Transition from inflammation to proliferation: a critical step during wound healing. Cellular and molecular life sciences : CMLS, 73(20), 3861–3885. https://doi.org/10.1007/s00018-016-2268-0
Barbosa, Danillo & Souza, Renato & Carvalho, Wellington & OLIVEIRA, MURILO & Carvalho, Paula & Cunha, Tereza & Arisawa, Emilia & Silveira, Landulfo & Villaverde, Antonio. (2013). Low-level laser therapy combined with platelet-rich plasma on the healing calcaneal tendon: A histological study in a rat model. Lasers in medical science. 28. 10.1007/s10103-012-1241-x.
Ozaki, G. A. T., Camargo, R. C. T., Koike, T. E., Garcia, T. A., Castoldi, R. C., Pereira, J. D. A. D. S., Constantino, C. J. L., & Camargo Filho, J. C. S. (2016). Analysis of photobiomodulation associated or not with platelet-rich plasma on repair of muscle tissue by Raman spectroscopy. Lasers in Medical Science, 31(9), 1891–1898. https://doi.org/10.1007/s10103-016-2067-8